
TUBA1A - associated tubulinopathy is a genetic condition caused by a change to a gene called TUBA1A . So far, most children with TUBA1A - associated tubulinopathy have been found to have developmental delay, altered brain formation and a small head. Epilepsy is also common. Many children have additional neurological symptoms that mainly affect muscle activity.
With an estimated 600 known cases cases worldwide, TUBA1A can feel isolating. But you are not alone. The TUBA1A Foundation connects families, shares resources, and fosters a sense of community. We believe that understanding and support can make a world of difference.
There is currently no cure for TUBA1A, but therapies and early interventions can help children reach their fullest potential. We’re here to guide you through available options and connect you with others who understand your experience.
TUBA1A - associated tubulinopathy is caused by specific changes (known as pathogenic variants) to a gene called TUBA1A (TUBA1A is an abbreviation of the gene’s full name, tubulin alpha-1A, hence the name tubulinopathy). The TUBA1Agene is located on the long ‘q’ arm of chromosome 12 in a region called 12q13.12 (see below).
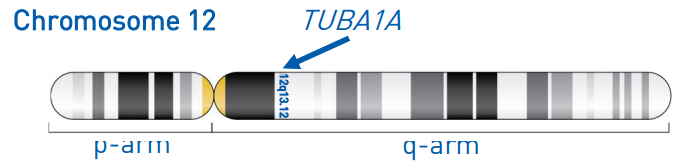
We have two copies of chromosome 12 in our cells, which means we also have two copies of the TUBA1A gene.
TUBA1A-associated tubulinopathy occurs when only one copy of the TUBA1A gene is affected. This is known as an autosomal dominant condition, meaning the change occurs on an autosome (any of the chromosomes numbered 1–22), and features can be present when just one copy of the gene is altered.
The TUBA1A gene provides instructions for making the TUBA1A protein. This protein is found in most cells but plays a critical role in brain development. It helps form structures called microtubules, which have many important functions—one of which is ensuring proper cellular organization and development.
We encourage families to reach out, ask questions, and share their stories. By coming together, we create a space where hope and resilience thrive.
Most children with TUBA1A - associated tubulinopathy
Other Possible features may include:
• Brain anomalies
MRI brain scans reveal a range of changes in the majority of children diagnosed with TUBA1A-associated tubulinopathy. The changes include underdeveloped or absent corpus callosum (the connection between the left and right hemispheres of the brain). Most children also have an abnormality of the ridges of the folding pattern on the surface of the brain (known as cortical malformation).
• Epilepsy
Many children with TUBA1A-associated tubulinopathy reported in the medical literature are known to experience recurrent seizures. Types of seizures vary and include generalized tonic-clonic seizures, infantile spasms and focal seizures.
• Other neurological features
Muscle tightness (spasticity) has been reported in a significant number of children with TUBA1A-associated tubulinopathy. A few children have also been found to have reduced muscle tone (hypotonia).
• Eye problems
Some children are also diagnosed with eye problems. These include nystagmus (involuntary ‘wobbly’ eye movement), squint (when eyes do not properly align, also known as a strabismus) and underdevelopment of the optic nerve (optic nerve hypoplasia).
Development
• Physical Development
Children with TUBA1A-associated tubulinopathy usually show significant delay in reaching motor milestones. Some children learn to walk later than expected, some can stand and walk with support and some do not learn to walk at all.
• Intellectual Development and Learning
Children usually have severe learning difficulties or intellectual disability and may not be able to manage independently as adults. Many children need the support of a special education.
• Speech and language
Difficulties in speech and language generally mirror intellectual disability. Most children have severe speech and language difficulties and do not use meaningful words, and understanding is also usually limited.
• Behaviour
Most children generally have a friendly and pleasant personality. A few children with TUBA1A-associated tubulinopathy also have neurobehavioural difficulties such as autism or autistic-like features.
• Feeding
Feeding can be problematic for children with TUBA1A-associated tubulinopathy. While some children manage to eat with the help of a parent or carer, others receive their nutrition (and medication) via a gastric PEG (percutaneous endoscopic gastrostomy) tube, which is when a tube is fitted directly into the stomach via the abdominal wall.
TUBA1A is rare, but you are not alone. Support, therapies, and community can make a meaningful difference. We’re here to help you find answers, connect with others, and navigate this journey with hope.
Thank you for being part of the TUBA1A Foundation community. Together, we can build a future filled with compassion, understanding, and possibility.
Find answers and support for your family’s journey.
TUBA1A-associated tubulinopathy is a rare genetic disorder that impacts brain development. Each child’s experience is unique, and we’re here to help you understand what this diagnosis means for your family.
Diagnosis often starts with noticing developmental or neurological differences, followed by genetic testing. Your medical team will guide you through each step and answer your questions.
You’re part of a caring community. We offer resources, peer connections, and guidance to help you navigate therapies, daily life, and emotional support. Reach out to connect with others who understand.
Many children benefit from therapies like physical, occupational, and speech therapy. These can help with movement, communication, and daily skills. Your care team can recommend what’s best for your child.
There is currently no cure, but research is ongoing. Supportive care and therapies can make a real difference in your child’s quality of life.
Support families and research by donating, volunteering, or sharing your story. Every action helps build a stronger, more hopeful community.